The incredible story of how plasma donations help patients
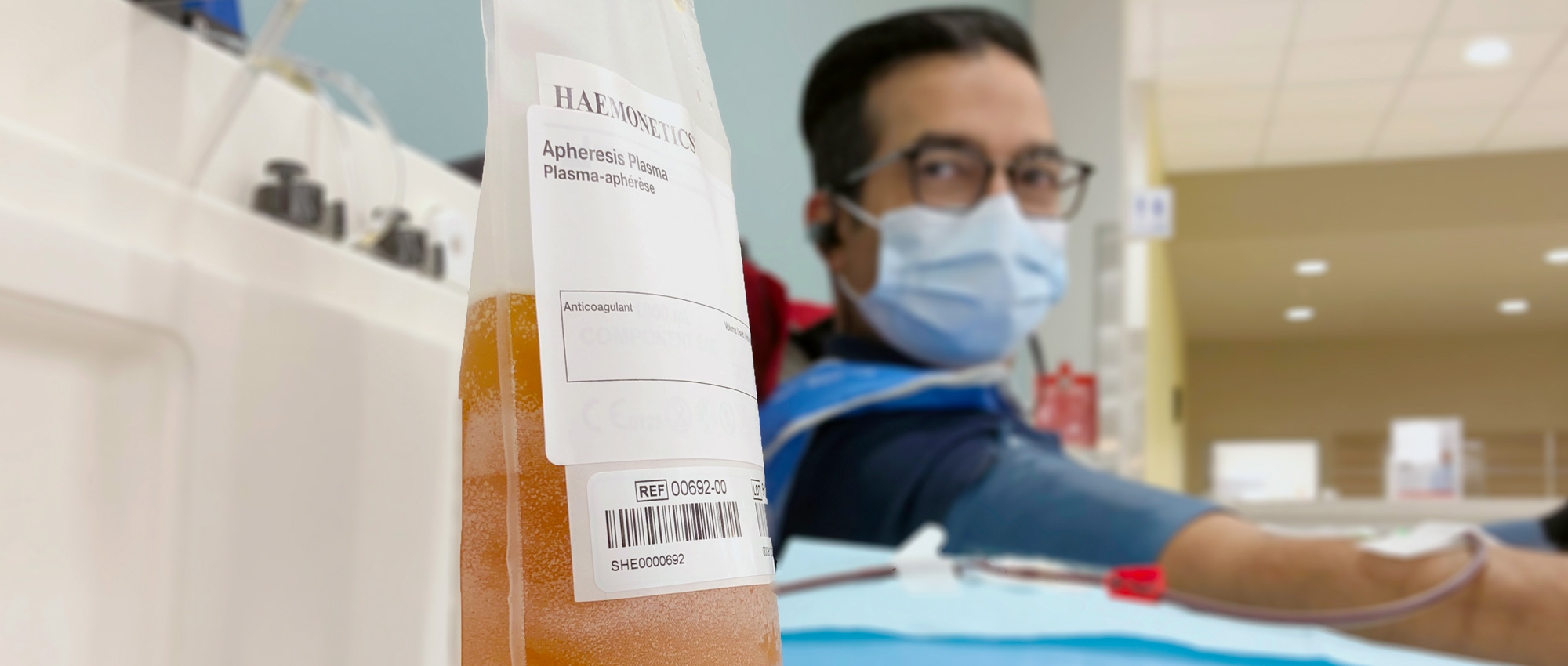
This straw-coloured component of blood is the source material for lifesaving medications. And patient need is soaring.
Ron Shivji of Calgary, Alta. has donated plasma hundreds of times.
Ask any person for a single word to describe “blood” and chances are, they’ll pick a colour: red. But did you know that red blood cells make up less than half your blood volume? In fact, the blood coursing through your blood vessels is mostly comprised of a pale yellow component called plasma.

When a donation of whole blood is spun in a centrifuge, the different components become visible in layers. Plasma, the straw-coloured component, makes up most of the volume. (Photo taken prior to the COVID-19 pandemic)
This pale liquid is just as vital to saving lives as the red cells. Blood plasma can be transfused directly to patients with liver failure, severe infections or serious burns. But where demand for blood plasma is really soaring, in Canada and around the world, is in the manufacture of specialized products for immune deficiencies, bleeding disorders, devastating autoimmune diseases and more. To make these products, donations are pooled and “fractionated,” a process that separates and extracts specific proteins from the plasma mixture. A single dose of some plasma protein products may contain proteins from more than a thousand different donors.
Expanding plasma donation to be more inclusive
This video was filmed prior to the COVID-19 pandemic.
To meet the needs of Canadian patients who rely on these products, we are working to substantially increase collection of plasma. But there’s a challenge. While Canadian Blood Services does obtain plasma from donations of whole blood, and has done so for decades, we cannot meet sharply rising demand through this method alone. To do so would lead to an oversupply of red cells from our generous donors.
Plasma donation gets a boost from Sikh Nation
The answer is greater reliance on plasmapheresis: a process for donating only the plasma portion of the blood, by using an apheresis machine. The machine returns red cells and other blood components to the body during the donation (as you can see in the video above). This allows plasma-only donors to give much more frequently than whole blood donors ― as often as once a week, compared with once every 2-3 months for whole blood. And with each sitting, they may also donate as much as three times more plasma than would be contained in a single donation of whole blood. Our bodies are constantly making the components of plasma and can replace them quickly.
1,000 plasma donations and counting in Charlottetown, P.E.I.
Plasma donors become ‘Friday Friends’ in London, Ont.
Shannon Morrison donated plasma on the first anniversary of the opening of the plasma donor centre in Sudbury, Ont., in Aug. 2021. Her son Heydan receives a medication made from plasma.
Plasma donation an easy, efficient way to serve community
The efficiency of plasma donation is precisely what motivated Ron Shivji, a father of two in Calgary, Alta., to switch from donating blood to donating plasma about 15 years ago.
“I work in the supply chain field, an area that deals with efficiencies,” says Shivji, who is now approaching his 500th plasma donation. “And I thought, well, if I can donate frequently, and it’s equivalent to three whole blood donations, why don’t I do that?”
The regular commitment appealed to him as well. As an Ismaili Muslim, Shivji grew up in a family and community that prioritizes service to others. He views his Friday plasma donation appointments as the equivalent of a weekly volunteer duty.

Ron Shivji of Calgary, Alta., has been donating plasma regularly for about 15 years.
“My general philosophy is that the world would be a better place if everyone did something for someone else,” he says.
But unlike some other volunteer opportunities, plasma donation is a predictable time commitment, Shivji notes. And that’s appealing. Within 90 minutes of walking into the donor centre, he’s finished for the week.
“They say thank you, you get your cookies and your drink, and you leave. Your commitment is done, yet you’ve done so much to help others,” Shivji says.
Understanding the motivation behind plasma donation
Canadian plasma donors helping Canadian patients
Every single one of Shivji’s donations is used to help a patient somewhere in Canada. After testing, his plasma donations travel with others from Canadian Blood Services to a fractionator in the United States or Europe. The fractionator pools them to make essential medications, which are then shipped back to us for delivery to Canadian hospitals.

Medications made from plasma are stored at Canadian Blood Services facilities such as this one in Brampton, Ont. before delivery to hospitals. (Photo taken prior to the COVID-19 pandemic)
In order to meet the needs of hospitals and patients across the country, Canadian Blood Services also buys plasma protein and related products on the global market. But the COVID-19 pandemic has also driven home for everyone the risk of relying too heavily on medications and other essential items sourced abroad.
Plasma security and sustainability: learn more
“At the beginning of the pandemic, plasma collection in the U.S. dropped significantly,” says Dr. Sylvain Grenier, a pharmacist and director of Canadian Blood Services’ plasma protein and related products formulary program.
That drop had implications for the production of immunoglobulin, the plasma protein product in greatest demand worldwide. For some critical immune deficiencies, it is the only treatment available.
“We are dealing with conditions that are life-threatening. For these patients, immunoglobulin is absolutely required,” Dr. Grenier says.

Sylvain Grenier is a pharmacist and director of Canadian Blood Services’ plasma protein and related products formulary program. (Photo taken prior to the COVID-19 pandemic)
Fortunately, Dr. Grenier says, by working with pharmaceutical manufacturers, government partners and hospitals to optimize the management of plasma-derived products inside our supply chain, Canadian Blood Services was able to meet the needs of all patients in those difficult early days of the pandemic, and we continue to do so. But we’re also looking to the future, and how our donors in Canada can help us meet the rapidly growing demand for immunoglobulin in particular.
“Year over year, we’ve been seeing an increase in usage of immunoglobulin of approximately eight per cent,” explains Elizabeth Stucker, Canadian Blood Services’ director of strategic planning and integration for plasma operations.
“And there is some recent evidence to suggest that the growth in demand will continue for the next several years. So every year, we’ll need to collect more plasma than we did the year before.”
This is our most important reason for welcoming more and more plasma donors to Canada’s Lifeline. In Aug. 2020 we opened our first standalone plasma donor centre in Sudbury, Ont., followed by two others in Lethbridge, Alta., and Kelowna, B.C. More new plasma donor centres are planned for the Ontario cities of Ottawa and Brampton. In the meantime, we continue to welcome veteran plasma donors like Ron Shivji, as well as new ones, at our established sites in other cities across Canada.
How to donate plasma at our sites across Canada

Ian Harrop of Calgary, Alta., who donated whole blood before becoming a regular plasma donor in the 1990s, celebrated his 600th donation with a skydive.
When you donate plasma, you never know who you might be helping. Some of Ron Shivji’s hundreds of donations could even have helped a fellow Calgarian, Dean Lower.
Four years ago, Lower was a healthy 51-year-old financial industry executive when he developed chronic inflammatory demyelinating polyneuropathy (CIDP), a disorder in which the body’s immune system attacks the nerves. When he was first admitted to hospital, doctors initially diagnosed him with Guillain-Barré syndrome, the acute form of the illness, and stabilized him with immunoglobulin treatments over seven days. But a few weeks later his symptoms returned.
“I went back in and started a 60-day journey, with a stop in ICU,” Lower recalls. “They told my wife I most likely wouldn’t survive ICU, and that if I did I would most likely be quadriplegic. Or best-case scenario, paraplegic.”

Dean Lower was treated with medication made from donated plasma for a condition called chronic inflammatory demyelinating polyneuropathy (CIDP).
Plasma donors helped Lower avoid that outcome. During that second hospital stay, he received a large dose of immunoglobulin as well as treatments with albumin. Albumin is a plasma protein with a long history of use. It was successfully removed from whole plasma in the early 1940s, after Dr. Edwin Cohn, a Harvard University biochemist, was asked to identify a stable blood derivative or substitute that could be stockpiled and shipped anywhere in the world, to treat shock in injured soldiers. Dr. Cohn and his colleagues not only helped save the lives of many soldiers in the Second World War, including at Pearl Harbor, they pioneered plasma fractionation, paving the way for the many other products ― including immunoglobulin ― that are saving lives today.
Lower’s treatment involved the removal of his own plasma and the replacement of that fluid with an albumin solution, a process called “plasma exchange.” As he lay in hospital immobilized, doctors kept giving him that treatment until a breakthrough occurred.
“I literally woke up in the morning and my thumb moved, for the first time in six weeks roughly,” Lower says. “And in the afternoon my other thumb moved. The next morning, I could make my hand move to operate the TV remote.”
Soon he was able to wiggle his toes as well. As Lower’s function continued to dramatically improve, his medical team stopped the plasma exchanges after 26 treatments.
“It was miraculous how my body came back, and it was this life-giving plasma,” says Lower.

Dean Lower of Calgary, Alta., regained his ability to move after treatment with products derived from plasma, a component of blood.
While most people have never heard of plasma exchange, Lower’s neurologist at Calgary’s South Health Campus says that along with immunoglobulin, it is crucial for many of his patients.
“Our plasma exchange clinic is a very busy place,” says Dr. Christopher Hahn, clinical assistant professor in the University of Calgary’s Department of Clinical Neurosciences. “Someone is getting plasma exchange every day.”
And as is the case with some immune deficiencies, for some of the auto-immune neurological conditions Dr. Hahn treats, plasma-derived treatments are the only option.
“For Guillain Barré syndrome, it’s really IVIg (intravenous immunoglobulin) or plasma exchange,” he says. “There’s nothing else. If we didn’t have those products, we would lose our ability to treat a condition that is not uncommon. And for some of the other conditions, IVIg and plasma exchange are better tolerated, have less side effects than some of the other medications we can use.”
Plasma donors helped get Lower through the darkest hours of his illness. Even after leaving hospital the second time, he received many more immunoglobulin treatments before qualifying for a newer drug that targets a specific antibody. He’s now living an active life. Last winter he went skiing for the first time since his diagnosis. And on a July hike with his wife at Moraine Lake, amid stunning views of the Rocky Mountains, his thoughts turned to plasma donors, without whom the adventure would have been impossible.
“We got there early in the morning and we just walked along the lake. It was so quiet and peaceful and just so beautiful,” Lower remembers. “And I thought, ‘I wouldn’t have been able to walk this’. Even in a wheelchair, we wouldn’t have attempted that trail.”

Dean Lower is back to an active life thanks in part to plasma donors. They have been essential to his treatment for chronic inflammatory demyelinating neuropathy, and could be again in the future.
Lower is also mindful of the fact that with his condition, things could change in a heartbeat. In a few years, he expects to need to be weaned from the drug that is currently helping him, and it’s possible he’ll need to resume plasma exchange treatments. It comforts him to know that because of donors, that treatment will be available. And he’s so thankful for the second chance they’ve already given him.
“Life is measured in moments,” Lower says. “We celebrated my son’s 18th birthday in March and I got to be here for that. So I’m grateful.”
Plasma donations are used to make products that help patients with devastating immune deficiencies, neurological conditions and more. And the need for these products is rising sharply. To donate plasma, use the GiveBlood app, book online at blood.ca or call 1 888 2 DONATE. For more information about Guillain Barré syndrome and CIDP, visit the GBS/CIDP Foundation of Canada.