Nancy Heddle – integrating expertise to make transfusion safer
Wednesday, November 23, 2016 Dr. Kendra Hodgkinson
Meet Nancy Heddle, an adjunct scientist with Canadian Blood Services and a professor at McMaster University. She has a background in health sciences, with a M.Sc. from McMaster and a certification from the Canadian Society of Medical Laboratory Science. Her main expertise is in blood banking, clinical epidemiology and biostatistics.
Nancy Heddle is the research director of the McMaster Centre for Transfusion Research (MCTR) and also directs the Quality Essentials for Safe Transfusion (QUEST) Hamilton-Niagara program.
Somehow, she also manages to find the time to do her own research, which focuses on improving evidence-based decision-making in transfusion clinical practice. Her interests span many areas, including transfusion outcomes, clinical thresholds for transfusion, pathogen reduction in platelet transfusions, and treatments for blood disorders.
Red blood cell storage time – how long is too long?
There is no question that blood transfusions save lives. Whether some blood products lead to better patient outcomes than others, however, has been the subject of much discussion. Nancy Heddle has been at the forefront of investigating some of the big questions around the use of blood products – like storage time and best manufacturing processes – and their link to transfusion outcomes.
A large international study led by Nancy Heddle recently generated a lot of buzz. You may have seen this CBC article about the effects of red blood cell storage time on transfusion outcome. The study was published October 24 in the New England Journal of Medicine and was highlighted in this month’s Research Unit on the blood.ca website.
ResearchUnit: Older blood as good as new: no harmful effects of storage time before transfusion
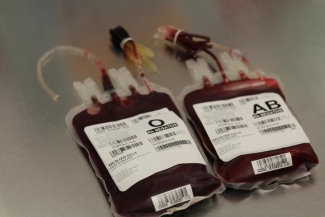
In North American blood banks, red blood cells are stored for up to 42 days between collection and transfusion. What happens during those 42 days? Red blood cells remain metabolically active and slowly use up their energy stores, causing gradual molecular changes in the cells. Some cells burst, releasing metabolic chemicals into the storage bag. These changes are collectively referred to as the red blood cell “storage lesion.”
But does this “storage lesion” actually affect patient outcome? Researchers confirmed in the 1970s that blood stored for up to 42 days is safe, but about ten years ago, several studies raised concerns that transfusion outcomes might be worse when blood is stored for more than two weeks.
To address these concerns, Nancy Heddle and her collaborators at six hospitals around the world (Canada, the United States, Australia and Israel) initiated the Informing Fresh versus Old Red Cell Management (INFORM) trial. In this study, patients requiring transfusion were randomly assigned to receive the freshest-available or the oldest-available red blood cell units, then transfusion outcomes were assessed by medical staff.
The INFORM trial researchers found that, in fact, older blood is just as good as newer blood; patients transfused with the older blood did not have a higher mortality rate than those given newer blood.
With this work, Nancy Heddle and her collaborators have helped reassure clinicians and patients that no harm will come from using blood that is several weeks old, as long as it is stored appropriately and remains within the current 42-day storage limit.
This kind of research is important to ensure that Canadian Blood Services is following the best possible procedures to maximize the safety and effectiveness of our blood products. We are proud to have talented scientists like Nancy Heddle on our research team.
The ability to link donor, blood manufacturing and storage characteristics with patient outcomes has the potential to radically change how clinical practice is informed by research and large data analytics. Earlier this year Nancy Heddle also found some associations between manufacturing processes and patient outcome. Read more
Congratulations to Nancy Heddle
The AABB, an international, not-for-profit association dedicated to improving patient outcomes in transfusion medicine and cellular therapies, recently recognized Nancy Heddle’s many contributions to clinical research with a prestigious award: the Emily Cooley Memorial Award and Lectureship. This award “recognizes an individual who has demonstrated teaching ability and has made a major contribution to the field of transfusion medicine or cellular therapies”.
Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
While blood transfusion is safer now than ever before, scientists continue to look for ways to reduce risk and ensure the healthiest possible outcomes for patients. A unique collaboration between Canadian Blood Services, The Ottawa Hospital and Université Laval has led to some interesting and...
Researchers show that some methods used in the manufacturing of red blood cell units may be less damaging to the cells, which could reduce adverse reactions in transfusion recipients. This work may impact the future of how blood is collected in North America and around the world.

