Aliquot (al – i – quot) – 1. a portion of a larger whole, especially a sample taken for chemical analysis or other treatment; verb 2. divide (a whole) into aliquots; take aliquots from (a whole).
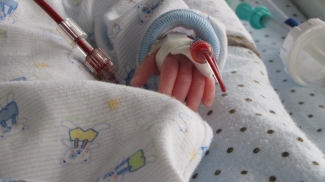
Dr. Chantale Pambrun is an associate medical director at Canadian Blood Services, currently working at our Head Office in Ottawa. Previously she worked as the medical director of the laboratory at the IWK Health Centre – a women’s and children’s hospital in Halifax. While at IWK, Dr. Pambrun provided irradiated blood products for neonates and encountered the challenge of reducing donor exposure in neonates. Every unit of blood represents a donor exposure. By splitting up a single unit to be transfused over several days to the same neonate, there is reduction in exposures as well as a reduction in the wasted blood. A unit is generally 250 ml and a neonate generally requires less than 50 ml.
As a safety measure to reduce the possibility of transfusion-associated graft versus host disease in at-risk recipients, cellular blood products are irradiated.
Because some hospitals, like the one Dr. Pambrun was working at, do not have the means to irradiate products prior to transfusion, products are irradiated at Canadian Blood Services and delivered to hospitals. To split up a single unit, the blood bag is then spun off at the hospital, and split into smaller portions (called aliquots) prior to use in a neonatal transfusion. Dr. Pambrun was curious about the impact their spin off process had on these products -- what are the levels of potassium and hemolysis, for example. She wanted to know: what’s in the aliquot?
It was at a Canadian Society for Transfusion Medicine (CSTM) conference when Dr. Pambrun found herself in discussion with colleagues and experts who agreed that the question was a good one — the idea to study the aliquot and answer the questions Dr. Pambrun had about impact on the red cells was born.
“What I really wanted to know was what is in the aliquot,” says Dr. Pambrun. “We decided to evaluate something that we are already doing in clinical practice, to help inform what we're doing and change our process, if necessary. In a hospital setting, we don't have the ability to test all of the things that we are able to test in a study.”
“There are a whole bunch of questions that we have the opportunity of answering because our clinical colleagues know that Canadian Blood Services has the technical resources to do these kinds of studies. These are not just about academic interest but they really aim to inform policy and our interpretation and application of standards.” says Dr. Jason Acker, a Canadian Blood Services’ scientist at the University of Alberta.
“We're fortunate to have great relationships between the research labs — our Centre for Innovation facilities and experts — and the transfusion medicine and science community in Canada.”
From previous studies into irradiation, Dr. Pambrun knew that while irradiation damages the troublesome white cells that remain in the product, it can also damage the red blood cells. Guidelines are in place to optimize red blood cell quality while ensuring maximum white blood cells damage. But she wanted to know more about the impact of preparing an aliquot from an irradiated spun unit, as was occurring in their hospital.
The study was done in collaboration with our blood for research facility (netCAD) and Dr. Dana Devine’s lab at the Centre for Blood Research in Vancouver.
Findings were recently published in the journal Transfusion: Supernatant reduction of stored gamma-irradiated red blood cells minimizes potentially harmful substances present in transfusion aliquots for neonates.
“I was relieved to find out that at the end of the day what we were giving the neonates was safe. Safe in the sense that we were removing the potassium, we were removing the mannitol, we weren't distorting the cell morphology and impacting functionality of those red cells or their oxygen carrying capacity; which is what we're trying to give back to the neonate in the transfusion.”
The study showed that aliquots can be safely drawn from a single unit of blood, reducing waste and minimizing the donor exposure for newborns who require multiple transfusions. Finding out what's in the aliquot has shown that this current hospital practice is safe.
Further reading
Learn more about how to obtain blood for research. Learn more about funding opportunities for Canadian researchers.

Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration. Find out more about our research impact.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
Researchers show that some methods used in the manufacturing of red blood cell units may be less damaging to the cells, which could reduce adverse reactions in transfusion recipients. This work may impact the future of how blood is collected in North America and around the world.
Located in Vancouver, BC, near the University of British Columbia campus, our blood for research facility comprises a whole blood and apheresis donor clinic as well as a research and production laboratory.

