Knowledge synthesis forum highlights dedication of research teams and stakeholders, commitment of Canadian blood operators
Friday, July 31, 2020 Dr. Geraldine Walsh
With funding from Health Canada, Canadian Blood Services and Héma-Québec are supporting research to contribute to the establishment of adequate evidence-based research for alternative screening approaches for blood or plasma donors, which could evolve the current deferral policy for men who have sex with men (MSM) while maintaining the safety of the blood supply. The MSM Research Program funds 15 innovative research projects to generate evidence that is currently lacking.
The Canadian research efforts will contribute to a growing national and international body of knowledge on the topic, as other countries and jurisdictions also seek to advance their eligibility criteria for men who have sex with men.
Although many of the research projects are not due to complete until 2020 and 2021, in November 2019 Canadian Blood Services and Héma-Québec hosted a knowledge synthesis forum to bring stakeholders together and see where this research stands. The 2-day meeting allowed participants to connect the new pieces of evidence together and identify where gaps remain. A report detailing the research progress so far and providing an overview of the discussions at the forum is now available on blood.ca.
Read the Knowledge Synthesis Forum Report here.
As highlighted in the report, the multiple research teams represent a new Canadian network of collaborators with complementary expertise that is set to deliver important data. Together, the teams will help answer key questions as blood operators move towards making blood donor eligibility criteria as minimally restrictive as possible while maintaining the safety of the blood system. These questions are focused around three main themes: acceptability, safety and feasibility.
- Is the change acceptable? Would it be acceptable to gay, bisexual and other men who have sex with men? Would it be acceptable to recipients of blood and blood products? Would it be acceptable to Canadians? Will it address underlying concerns about discrimination?
- Is the change safe? Would the change impact the safety of the blood supply? How would it impact the risk of infection from a blood transfusion?
- Is the change feasible? What are the potential impacts of the change? How would it impact the sufficiency of the blood supply? Can it be put into operation?
Blood donation and men who have sex with men
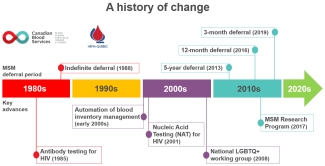
In Canada, men who have sex with men were first indefinitely deferred from blood donation in 1988 when they were noted to be a particularly high-risk population for HIV/AIDS. Advances in the way blood operators manufacture and tests blood products and evidence such as epidemiological and safety data supported a change to a time-based 5-year deferral in 2013, then a 12-month deferral in 2016. As of June 2019, men are eligible to donate blood if it has been more than three months since their last sexual contact with a man.
As results from the research projects continue to emerge over the coming months, we will share results and related activities here on our R.E.D. blog. To keep updated on this and other research and education activities at Canadian Blood Services, subscribe to our Research and Education Round Up Newsletter.
Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration. Find out more about our research impact.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
New publication: Donor deferral policies for men who have sex with men: past, present and future
Canadian Blood Services has recently made progress on several fronts that may further evolve the eligibility criteria for men who have sex with men. This includes supporting more research projects as part of the MSM Research Grant Program and working to reduce the waiting period from one year to three months based on the latest evidence.
As work gets underway, the lead investigators in one of fifteen funded MSM Research projects, discuss the significance of consultation and collaboration to their research, and explain the anticipated impacts and feasibility of introducing alternative donor eligibility screening criteria for source plasma.