Kidney Paired Donation – powerful program reaches significant milestone
Tuesday, June 20, 2017 Jenny Ryan
500 transplants made possible thanks to the selflessness of living organ donors and kidney paired exchange
As of May 2017, more than 500 kidney transplants have occurred across Canada through the Kidney Paired Donation program. These are transplants that may otherwise have not occurred.
The Kidney Paired Donation program – launched in 2009 – is a perfect example of how interprovincial health systems work together to forge success beyond provincial borders and improve access to transplants for patients.
The success of this program can be attributed to the selflessness of the more than 500 individuals who have stepped forward to be living organ donors. Kudos to the truly altruistic non-directed anonymous donors (willing, living donors without a specific intended recipient) who make domino kidney exchanges possible.
A recent story on CBC showcases this program and the impact it can have on patients waiting for a transplant and their families.
Here is a bit more information about this program, gathered from Kathy Yetzer, Associate Director of Living Donation and Transplantation and Dr. Kathryn Tinckam, a transplant nephrologist at the University Health Network in Toronto, Canada, and a Medical Advisor in Transplantation to Canadian Blood Services.
What is the Kidney Paired Donation program?
The Kidney Paired Donation program is a living donation program that finds and facilitates medically compatible kidney transplants through chains of donor exchanges from medically incompatible pairs.
How did the Kidney Paired Donation program come to be?
Often individuals are unable to donate to someone they know because testing has determined that they are not medically compatible with the transplant candidate, and the kidney would therefore be rejected.
In 2009, Canadian Blood Services, in collaboration with transplant programs across the country, established a Kidney Paired Donation program for Canada.
Working in collaboration with the provincial living donation programs, the KPD program serves patients who have a willing living donor with whom they are not medically compatible by finding another pair with whom they can swap donors so both patients receive a transplant.
How does the Kidney Paired Donation Program work?
The registry contains medical information about incompatible pairs of donors and transplant candidates from across Canada and identifies pairs that might be able to exchange kidneys. From there, it’s a matter of finding a suitable exchange and creating “chains” of matching donors and recipients. There are different types of donor and recipient chains: some are straightforward swaps (called a “paired exchange”), some involve multiple donor–candidate pairs (called a “closed chain”), and some include a nondirected anonymous donor and a person on the waitlist (called a “domino chain”).
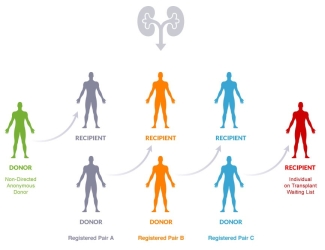
The program is supported by a sophisticated web-based software to optimize the number of donors and transplant candidates matched through the Kidney Paired Donation program.
A matching algorithm is run three times a year to compare the medical information on all the pairs and non-directed donors in the Registry and identifies kidney transplant opportunities.
Non-directed donors greatly increase the number of available matches. This selfless act of giving by non-directed donors has meant that as of June 8, 2017, 309 of the 505 transplants completed have been through domino exchanges.
What does the Kidney Paired Donation program do for patients?
Kidney transplantation is the preferred therapy for patients with kidney failure. Compared with dialysis, transplantation offers significantly longer life expectancy, a better quality of life, considerable cost avoidance per patient to the health care system, and an increased likelihood that the patient will remain employed.
Transplantation of a kidney from a living donor is advantageous to the recipient.The kidney lasts, on average, 25 per cent longer compared to a deceased donor kidney.
The added benefit to this approach is that patients transplanted through kidney paired donation are not added to the waitlist and this then shortens the waitlist and wait time for those patients who are dependent on receiving a deceased donor transplant.
The Kidney Paired Donation program significantly expands access to potential donors for all Canadians with an incompatible donor; every patient who receives a living donor transplant comes off the deceased donor waitlist and thereby decreases the demand on the waitlist for others.
Who can become a living kidney donor?
Any adult who is in general good health can be assessed to become a living kidney donor. If the donor wishes to donate to a friend or family member (a transplant candidate), medical assessments are conducted to determine whether the donor is a suitable match for the recipient. With a compatible match, the directed donation can proceed through the provincial program.
If the donor is not a match for their friend or family member, they may be able to help the transplant candidate find a matching donor through the Kidney Paired Donation program.
Further reading
- Read more about Kidney Paired Donation on blood.ca
- Highly Sensitized Patient program milestone
- Transplantation science has come a long way
- Canadian ingenuity enhances tool used to estimate patient access to life-saving transplants
Learn more about organ and tissue donation and register your intent to donate, visit organtissuedonation.ca
Canadian Blood Services and Organ and Tissue Donation and Transplantation
Canadian Blood Services works with the Organ and Tissue Donation & Transplantation community to improve national system performance. We do this through the development of leading practices, professional education, public awareness and data analysis and reporting. We also manage clinical programs that support interprovincial sharing of organs.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
Two hundred and fifty donations facilitated through the Highly Sensitized Patient program We are pleased to share the news of an exciting milestone for the Highly Sensitized Patient program. As of Monday, Aug. 22, 2016, there have been 250 transplants since going live in October 2013! The Highly...