A new process for red blood cell washing
The Evidence
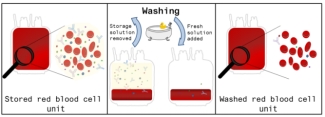
In 2011, Canadian Blood Services began a multi-year study to investigate and implement a washing process using a sterile “closed” system that allows storage after washing for up to 7 days in a nutrient solution. The researchers determined the best storage times for washed products. They optimized the process to ensure washed cells would meet all requirements for all patients. The washing system was introduced in October 2013 and researchers continued to monitor the impact on safety, efficacy and use, by examining hospital data. The quality of cells washed with the new system was equal to or better than those washed with the old system. Adverse transfusion reaction rates did not change, occurring in 0.15 per cent of transfusions both before and after implementation. The findings were published in 2016.
The Impact
These “bench to bedside” studies allowed the implementation of a superior washing system that ensures patient safety and improves product utilization. The longer storage time after washing reduced red blood cell discards due to expiry from approximately 4 per cent of washed units before implementation to less than 1 per cent after implementation, resulting in estimated savings of $17,500 per annum.