Breakthrough brings universal blood a step closer to reality
In brief...
An improved enzyme can efficiently cleave the antigens on red blood cells that determine blood type. This helps open the door to ‘making’ universal blood.
The red blood cell can have one or a combination of A, B and O antigens and each blood type is either Rh positive (the D antigen of the Rh group is present) or negative (the D antigen is absent), resulting in eight major blood types (A, A-, B, B-, AB, AB-, O and O-). In a way, antigens are similar to flags on a flag pole — each antigen being a different type of flag that the immune system can recognize and react to. Imagine the flag representing Type A is blue, and the flag representing Type B is yellow. Type AB red blood cells fly both blue and yellow flags. A and B antigens have an attachment that is absent from Type O red blood cells, so Type O is a flag pole missing its flag.
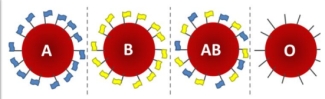
People with O negative blood are considered "universal donors". Just like the imaginary Type O flag pole, O negative blood lacks the antigen that can trigger an immune response. This means O negative blood can be safely transfused into any recipient. The extra attachment on the antigens of Type A and B blood can be removed (or cleaved) by enzymes. This results in red blood cells with shorter, non-specific antigens similar to those found on universal Type O red blood cells. Naturally occurring enzymes can cleave A and B antigens; however impractically large amounts of these enzymes would be needed to process all the red blood cells in just one unit for transfusion.
What did the researchers do?
Researchers at the University of British Columbia in Vancouver set out to engineer an enzyme with improved ability to cleave A and B antigens. Beginning with an enzyme from the bacterium Streptococcus pneumonia, the researchers altered a wide range of the enzyme’s building blocks (amino acids) to search for that special combination that had the highest antigen cleavage activity. This approach is referred to as “directed evolution”. After each alteration, the researchers tested the enzyme’s ability to cleave the antigens. This sequential process honed in on the altered enzymes with the best cleavage ability and these combinations were selected for further improvement. The researchers used a technique called ‘crystallization’ to solidify the enzymes and look at their structure. Whether the antigens had been cleaved was tested using antibodies that bind to the antigens and fluoresce (emit light) so the antigens can be seen using a microscope.
What did the researchers find?
Based on knowledge of the enzyme structure and activity, the researchers conducted five rounds of alterations of the enzyme. By careful selection they were able to engineer an enzyme that has a 170-fold increase in its ability to cleave antigens on the surface of a cell. The shortened antigens are not exactly like those of Type O blood but are comparable.
How can you use this research?
Blood transfusions are an essential part of care for thousands of Canadian patients each year. Managing the blood products necessary to ensure every patient has access to the right product at the right time is an everlasting cycle of supply and demand. Naturally, universal O negative blood is in high demand as it can be transfused in emergency situations when there is no time to test the patient’s blood type. For that reason, 12 per cent of hospital requests Canadian Blood Services receives are for O negative blood; however only about seven per cent of Canadians have this blood type. While Canadian Blood Services O negative donor base is above the national average at 10 per cent, this donor group is consistently asked to donate every 56 days to keep up with hospital demand.
This is difficult to sustain and results in an imbalance between the supply and demand for O negative blood. ‘Making’ Type O blood using other red blood cells could help reset the balance. This research improved a naturally occurring enzyme in such a way that a much smaller amount of the enzyme is needed to cleave a much higher percentage of antigens. This brings us one step closer to a practical method for making a blood type that can be transfused into most people.
Will blood typing become a thing of the past? Blood typing is here to stay for the foreseeable future. More ‘directed evolution’ is needed to further improve the enzyme and to ensure conversion of the entire red blood cell unit for transfusion. Beyond that, it still must be shown that red blood cells treated with the enzyme will not trigger an immune response. This is necessary before manufactured ‘universal blood’ could be used in hospitals. While more research is needed, the development of this enzyme brings the exciting possibility of creating universal blood closer to realization.
About the research team
This research was led by Dr. Stephen G. Withers, a professor in the departments of chemistry and biochemistry and a member of the centre for high-throughput biology at the University of British Columbia, Vancouver, BC and Dr. Jayachandran N. Kizhakkedathu, an associate professor in the department of pathology and laboratory medicine, an associate member of the department of chemistry and a member of the centre for blood research at the University of British Columbia. The research was conducted in collaboration with the department of biochemistry and microbiology at the University of Victoria, Victoria, BC and the centre de recherches sur les macromolecules végétales, Centre National de la Recherche Scientifique, Grenoble, France.
This research unit is derived from the following publication(s)
[1] Kwan DH, Constantinescu I, Chapanian R, Higgins MA, Kötzler MP, Samain E, Boraston AB, Kizhakkedathu JN, Withers SG: Towards efficient enzymes for the generation of universal blood through structure-guided directed evolution. J. Am. Chem. Soc. 2015; 137:5695-5705
Acknowledgements: This research was supported financially by Canadian Blood Services, funded by the federal government and the provincial and territorial ministries of health, and by the Canadian Institutes of Health Research (CIHR). Infrastructure support was from the Canada Foundation for Innovation, the British Columbia Knowledge Development Fund, the Canada Research Chairs program and the Michael Smith Foundation for Health Research (MSFHR). D.H.K. is a recipient of CIHR and MSFHR research trainee postdoctoral fellowships. R.C. is a recipient of a CIHR/Canadian Blood Services postdoctoral fellowship and a MSFHR postdoctoral trainee. J.N.K. is a recipient of a MSFHR career investigator scholar award. S.G.W. is a Tier-I Canada Research Chair in chemical biology. This ResearchUnit was prepared by Christa Klein, a graduate student affiliated with Canadian Blood Services’ centre for innovation.
Keywords: Antigen, blood type, enzyme, red blood cell, universal donor
Want to know more? Contact Dr. Withers at withers@chem.ubc.ca or Dr. Kizhakkedathu at jay@pathology.ubc.ca
Research unit is a knowledge mobilization tool developed by Canadian Blood Services’ Centre for Innovation