The 2019 Canadian Transplant Summit took place Oct. 15-19 in iconic Banff, Alta. Presented by the Canadian Society of Transplantation (CST), Canadian Blood Services and the Canadian Donation and Transplantation Research Program (CDTRP), this annual event is a unique opportunity to bring together medical professionals, scientists, patients and stakeholders of all interests in organ donation and transplantation from across Canada.
This community works together to foster a future which will increase access to organs, cells and tissues, and improve health outcomes for Canadians living with a transplant. The meeting was a key networking and knowledge exchange event that attracted more than 350 participants.
Highlights
As part of the opening keynote address on Oct. 16, the audience experienced two very diverse life-saving perspectives.
Winner of the 2012 Nobel Prize in Economics, Alvin Roth of Stanford University, presented the opening plenary titled “Kidney Exchange: an opportunity for cooperation in North America”, a look at the impacts of cross-border kidney sharing. Dr. Roth helped design the high school matching system used in New York City, and is one of the early founders and designers of kidney exchange in the United States, which helps incompatible patient-donor pairs find compatible kidneys for transplantation.
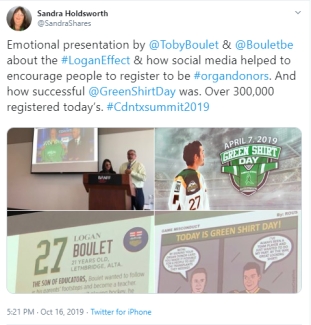
The parents of Logan Boulet, Toby and Bernadine, shared their perspective on organ donation and transplantation as a donor family. Logan Boulet made the decision to be an organ donor just weeks before his passing in the tragic Humboldt Broncos bus crash in April 2018. Inspired to register by his coach and mentor, Ric Suggit, who became an organ donor following his death in 2017, Logan registered his decision and took the wise and necessary step of sharing his decision with his family.
Logan’s legacy lives on and continues to inspire Canadians to register their intent to become organ donors. The first annual Green Shirt Day was held on April 7, 2019 in Logan’s honour. This annual tribute continues to raise awareness and honour the selfless gift that is organ donation.
A number of sessions throughout the conference provided insight into the work being done in Canada and internationally to push the boundaries of ‘higher risk’ donors, and especially to increase the uptake and usage of Hepatitis C (NAT positive) donor organs for healthy waitlisted patient.
On Oct. 17, during a lunch symposium, Sean Delaney, associate director of listing and allocation at Canadian Blood Services, brought his unique perspective as both transplant professional and as a kidney recipient (a generous gift from his brother), currently on the waitlist for a second kidney. His presentation was titled “Patient perspective on the marginal or high risk offer vs. waiting for a 'better' offer.”
Delaney, based in Edmonton, Alta., was part of building the original Kidney Paired Donation (KPD) program, as well as implementing the highly sensitized patient (HSP) interprovincial kidney sharing program. Together, the programs have produced more than 1,000 transplants for Canadian patients through interprovincial sharing. Most recently, he has been working to advance heart and liver sharing through the Canadian Transplant Registry.
Artificial intelligence and machine learning were hot topics at this meeting and the subject of a half-day workshop presented by the CDTRP.
On Oct. 19, a morning session shared further insight into living donation. Dr. John Gill with the University of British Columbia presented about costs incurred by living donors that present a barrier or disincentives to donation. Dr. Rahul Mainra, a transplant nephrologist in Saskatchewan, presented about the impact of kidney paired donation and the importance of ‘matchability’ for kidney paired donation and transplantation. Allison Hunt, who donated her left kidney to a total stranger after a snap decision made at a cocktail party, provided perspectives from an altruistic living donor.
The poster sessions brought great insight into the wealth and breadth of research underway across the field. Kathy Yetzer, associate director of living donation with Canadian Blood Services, presented a poster about key success factors for Canadian living kidney donation transplant programs. The findings show that performance success was most influenced by implementation of living donation evaluation efficiencies; engaging program stakeholders; broadening living donation identification and awareness strategies; access to quality assurance resources; increased living kidney donation transplant funding; and operating room availability.
Altogether, CST 2019 was great forum for knowledge exchange and to advance organ and tissue donation and transplantation in Canada. Kudos to the organizing teams at the Canadian Society of Transplantation, Canadian Blood Services and the Canadian Donation and Transplantation Research Program.
Learn more about CST 2019
Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration. Find out more about our research impact.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
Health professionals, patients, and policy makers gathered in Ottawa to discuss the future of transplantation in Canada at the Canadian Transplant Summit 2018 — October 16-20, 2018. The Canadian Society of Transplantation, Canadian Blood Services, the Canadian Donation and Transplantation Research...
Transplanting organs, tissue or stem cells from one person to another saves lives. It was not easy to figure out what facilitates a healthy and successful transplant though. Efforts over a long time reveal the complexity of the procedure and that very specific circumstances are required. As researchers’ understanding of the immune system improved, so did the success rate of transplants.
Five hundred kidney transplants made possible through national highly sensitized patient program