Why O-negative blood is critical in life-or-death situations
Fewer than one in ten people in Canada have O-negative blood, and their donations are crucial in emergencies
A trauma patient arrives at the emergency room. The medical team doesn't know her blood type or if she has any special blood requirements, and it will take at least 45 minutes to find out. But she doesn’t have that much time. She’s bleeding too much.
Thankfully, she can rely on the generosity of O-negative blood donors to keep her alive when every moment matters.
O-negative blood donors, sometimes called “universal blood donors,” are essential to saving the lives of patients whose blood type is unknown.
____________________________________________________________________________________
ARE YOU ELIGIBLE TO DONATE BLOOD? Find out now
____________________________________________________________________________________
“Every time a person is in a trauma or losing a lot of blood, we’re going to use O-negative blood till we know their blood type,” says Dr. Jeannie Callum, transfusion medicine specialist and hematologist at Kingston Health Sciences Centre and professor in the Department of Pathology and Molecular Medicine at Queen’s University.
“We will switch when we know it’s safe, but it takes about an hour to find out and that window is critical.”
Only 12 per cent of Canadian Blood Services donors are O-negative which means our inventory is frequently in short supply while demand is always high.
What is O-negative blood?
A person’s blood type is determined by protein and sugar molecules on their red blood cells.
“Our red blood cells have 360 protein and sugar decorations on their surfaces, called antigens, and among those 360 there are two really important antigens: ABO and Rhesus,” explains Dr. Callum.
The ABO system is composed of A and B antigens. If your blood has just one of the two, you’ll be type A or B, depending which antigen you have. Some people have both antigens, so their blood type is AB. If you have neither antigen, you’re type O.
The other most important system, the Rhesus or Rh system, involves a protein called the D antigen. If your red blood cells have the D antigen, you have a positive blood type. If they don’t, your blood type is negative.
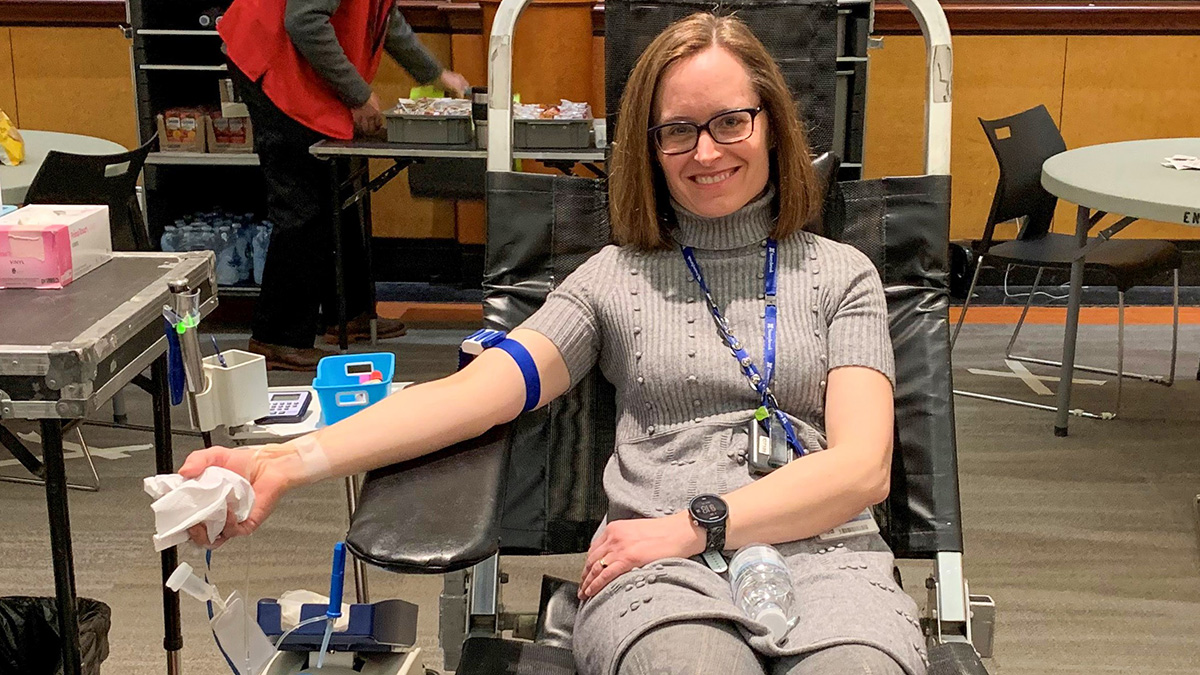
Dr. Jeannie Callum is a transfusion medicine specialist and O-negative blood donor.
How many people in Canada have O-negative blood?
Countries vary in terms of which blood types are most common. But in Canada, fewer than one in ten people have O-negative blood.
Blood type is inherited. So if you have a biological parent or sibling with O-negative blood, you might be O-negative as well. But you could have O-negative blood even if your parents have blood types A or B. When you donate blood for the first time, we’ll test and confirm your ABO type at every donation.
Why blood type matters
Our immune systems are designed to know what belongs in our body and what doesn’t. When recipients get blood containing antigens that don’t occur in their own blood, things can go very wrong.
“If you don’t have an antigen and someone puts blood containing that antigen into you, your immune system goes into attack mode and blows up those transfused blood cells,” says Dr. Callum.
“Your kidneys are likely to go into failure, you get really sick, and many patients in that situation will die."
Thanks to the availability of type-O blood and modern testing protocols, the above scenario is very unlikely to occur. In fact, the risk of ABO incompatible transfusion is estimated to be 1 in 354,000.
The D antigen is also very important because if a person with child-bearing potential is Rh-negative and receives Rh-positive blood, they will likely develop an antibody that could cause future pregnancy complications and losses.

Don't want to donate blood alone? Ask a friend if they want to go with you - they may even have O-negative blood!
O-negative blood is necessary for emergencies
In short, O-negative blood is critical because of what it doesn’t have: the A, B and D antigens, which can all trigger an immune response when the recipient isn’t a match. That’s why donations from people with O-negative blood can help people with any other blood type, and why O-negative blood is vitally important to emergency and critical patient care.
It’s also why Dr. Callum, who has O-negative blood herself, has made donating blood a priority.
“It’s a little magical to donate blood and know that about a week later your blood is in a patient somewhere and helping them feel better,” she says. “I feel it’s my duty to donate while I’m healthy and able. Especially because I know a lot of O-negative blood is used for emergency resuscitation and newborn babies.”




